SoCal's ICU capacity drops to 0% as overwhelmed hospitals struggle to cope with COVID surge

COVID-19 models plot dire scenarios for California hospitals
COVID-19 models project over the next four weeks the state’s hospitals could be overflowing with 75,000 patients — about five times the current level — and an average of 400 people will die every day.
LOS ANGELES - Southern California's intensive-care unit capacity dropped to 0% on Thursday, a day after Los Angeles County's health services director warned that the hospital systems were "under siege."
Hospitals are filling up so fast that officials are rolling out mobile field facilities and scrambling to hire doctors and nurses, while the state is distributing 5,000 body bags mostly to the hard-hit Los Angeles area.
RELATED: California ups order of body bags, reminding that COVID-19 remains deadly
According to state released data, SoCal's ICU capacity dropped from 0.5% on Wednesday to 0.0% by Thursday.
Los Angeles County's health services director Dr. Christina Ghaly warned on Wednesday that the increase in COVID-19 cases and hospitalizations will lead to "an increase in deaths in the days and weeks to come."
"I want to be very clear, our hospitals are under siege, and our models show no end in sight and the worst is still before us," Ghaly said.
LA County officials said Wednesday that two people are dying every hour as hospitals struggle to keep up with the surge of coronavirus patients.
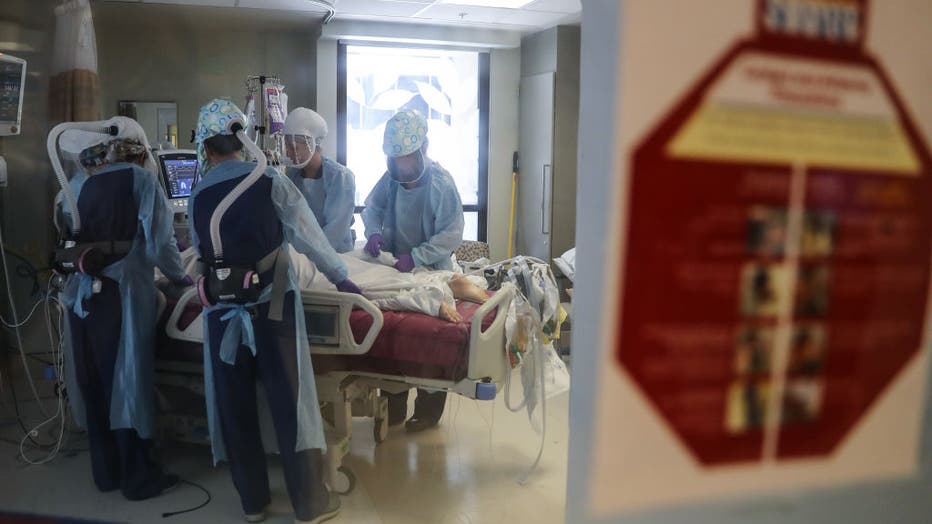
(Photo by Mario Tama/Getty Images)
"Today in Los Angeles County, let me be clear, we have a problem, and, at this point, all our hospital systems can do is brace for the days and weeks to come," Ghaly added.
California has seen coronavirus cases and hospitalizations soar in recent weeks.
In Orange County, mobile field hospitals were being set up in large trailers to assist in the influx of COVID-19 patients being admitted to hospital care. UCI Health is planning to add an additional 50-bed mobile field unit by Christmas.
RELATED: Orange County rolls out mobile field hospitals to handle surge in COVID-19 patients
The Orange County Health Care Agency on Wednesday issued an order suspending ambulance diversions for hospitals that take part in the 911 system, meaning that ambulances will no longer be redirected from one hospital emergency room to another when a hospital reaches capacity.
Dr. Carl Schultz, the agency's EMS medical director, said in a statement that hospital emergency rooms have become so overwhelmed due to the COVID surge that "almost all hospitals were going on diversion."
"Therefore, we temporarily suspended ambulance diversion. While this will place some additional stress on hospitals, it will spread this over the entire county and help to mitigate the escalating concern of finding hospital destinations for ambulances," Schultz said in a statement.
RELATED: Orange County suspends ambulance diversions as hospitals reach capacity
Jeremy Zoch, chief executive at Providence St. Joseph Hospital of Orange, said nurses, respiratory therapists and housekeepers have been taking extra shifts to help out during the crush. Registry and traveling nurses have come in and officials are talking to a nearby children’s hospital about using additional space to care for patients, he said.
"It has challenged us. So, every single one of our units that we have available to us, we’ve been redesigning them and utilizing them to care for COVID patients," Zoch told reporters. "It is really challenging us on the capacity front."
California health authorities reported Thursday a record 379 coronavirus deaths and more than 52,000 new confirmed cases.
The staggering new figures mean California has seen more than 1,000 deaths in the last five days and nearly 106,000 confirmed cases in just two days.
Many of the state’s hospitals are running out of capacity to treat the severest cases.
California’s pandemic death toll now stands at 21,860. The state has also seen the most cases in the nation with more than 1.7 million confirmed.
Get your top stories delivered daily! Sign up for FOX 11’s Fast 5 newsletter. And, get breaking news alerts in the FOX 11 News app. Download for iOS or Android.
Most California residents are under a stay-at-home order because of dwindling intensive care unit capacity where they live.
Southern California and the Central Valley — regions that together include 23 counties — had exhausted their regular supply of intensive care beds and many medical centers were already tapping into their "surge" capacity.
California is averaging more than 35,000 new reported coronavirus cases a day. Health officials estimate 12% of them — 4,200 — end up in hospitals.
The massive rise in infections began in October and is being blamed largely on people ignoring safety measures and socializing with others. More recently, health officials said they’ve seen cases stemming from gatherings during the Thanksgiving holiday and have pleaded with residents to avoid getting together with people from other households over Christmas and New Year’s.
RELATED: Unions for frontline workers call for 4-week shutdown in LA County in January amid COVID-19 surge
Hospitals administered the first Pfizer vaccines to health care workers this week as a pair of state advisory committees started making potential life-and-death decisions over who is next in line for the scarce inoculations. The committees are considering whether groups like teachers, farmworkers, grocery workers, ride-hailing drivers and news reporters should be among them.
On Wednesday, California announced the San Francisco Bay Area would join three of the state’s five regions already under a state-mandated stay-at-home order as ICU available beds dropped below 15%. The regions of greater Sacramento, the San Joaquin Valley and Southern California are already under Gov. Gavin Newsom’s order, which closes businesses including hair and nail salons and movie theaters and severely limits retail operations.
The Northern California region, which includes Humboldt, Lake and Mendocino counties, is not affected for now.
Many of the Bay Area’s counties had already applied the order as a precaution and those that hadn’t must now do so on Thursday.
Barbara Ferrer, the public health director for Los Angeles County said the transmission of the virus is rampant.
"We’re experiencing an explosive and very deadly surge," Ferrer said.
The Associated Press contributed to this report.

