Vaccination after COVID-19 infection gives 'hybrid' immunity to some, studies suggest
Some people who have previously been infected with COVID-19 and later received a vaccine may develop a powerful immunity to the virus and variants of it that emerge, recent research suggests.
These people may develop a "hybrid vigor immunity" to SARS-CoV-2, the coronavirus that causes COVID-19, and are likely able to fight off variants that evolve, according to immunologist Shane Crotty.
"When natural immunity to SARS-CoV-2 is combined with vaccine-generated immunity, a larger-than-expected immune response arises," Crotty wrote in a commentary published earlier this summer.
A study published last month by researchers at Rockefeller University found the combination of prior infection and vaccination broadened the strength of people’s immunity against a changing virus. The antibodies in these individuals were found to neutralize six variants of concern that were tested, including the delta strain.
"One could reasonably predict that these people will be quite well protected against most — and perhaps all of — the SARS-CoV-2 variants that we are likely to see in the foreseeable future," Paul Bieniasz, a virologist at Rockefeller University who helped lead several of the studies, told NPR.
Vaccinated survivors "can make antibodies that can recognize all kinds of variants even if you were never exposed to the variant," Crotty told the Associated Press last month. "It’s pretty sweet."
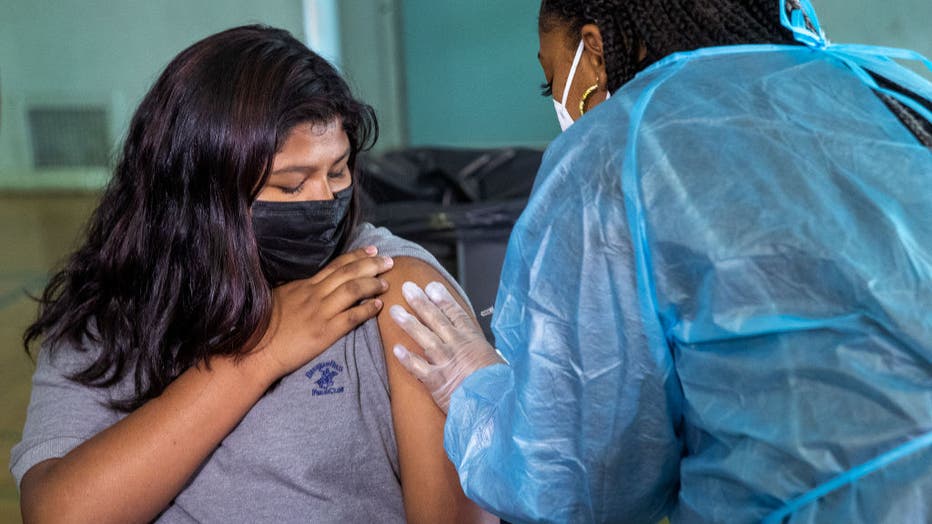
FILE - A student at San Fernando Middle School receives the first dose of the Pfizer-BioNTech COVID-19 vaccine from a licensed vocational nurse on Aug. 30, 2021, in San Fernando, California. (Mel Melcon / Los Angeles Times via Getty Images)
The U.S. Centers for Disease Control and Prevention has long encouraged those who have recovered from COVID-19 to get vaccinated. A study published last month shows survivors who ignored that advice were more than twice as likely to get reinfected.
Researchers studied Kentucky residents with a lab-confirmed coronavirus infection in 2020, the vast majority of them between October and December. They compared 246 people who got reinfected in May or June of 2021 with 492 similar survivors who stayed healthy. The survivors who never got vaccinated had a significantly higher risk of reinfection than those who were fully vaccinated, even though most had their first bout of COVID-19 just six to nine months ago.
A different variant of the coronavirus caused most illnesses in 2020, while the newer alpha version was predominant in Kentucky in May and June, said study lead author Alyson Cavanaugh, a CDC disease detective working with that state’s health department.
That suggests natural immunity from earlier infection isn’t as strong as the boost those people can get from vaccination while the virus evolves, Cavanaugh said.
RELATED: US COVID-19 deaths surpass 650,000 as delta variant fuels pandemic
The amount of natural immunity can vary from person to person, possibly depending on how sick they were originally. A Rush University study found four of 29 previously infected people had no detectable antibodies before they were vaccinated — and the vaccines worked for them just like they work for people who never had COVID-19.
The reason why some of the previously infected have such a robust response to vaccination has to do with how the immune system develops multiple layers of protection.
After either vaccination or infection, the body develops antibodies that can fend off SARS-CoV-2 the next time it tries to invade. Those antibodies naturally wane over time, experts say. If an infection sneaks past them, T cells help prevent serious illness by killing virus-infected cells — and memory B cells jump into action to make lots of new antibodies.
Those memory B cells don’t just make copies of the original antibodies. In immune system boot camps called germinal centers, they also mutate antibody-producing genes to test out a range of those virus fighters, according to University of Pennsylvania immunologist John Wherry.
The result is essentially a library of antibody recipes that the body can choose from after future exposures — and that process is stronger when vaccination triggers the immune system’s original memory of fighting the actual virus, Wherry said.
With the delta variant’s super infectiousness, getting vaccinated despite a prior infection "is more important now than it was before to be sure," Crotty said. "The breadth of your antibodies and potency against variants is going to be far better than what you have right now."
RELATED: 75% of US adults have received at least 1 dose of COVID-19 vaccine, CDC says
This story was reported from Cincinnati. The Associated Press contributed.



