'Crisis' situation: OC hospitals told to add space, cancel elective surgeries amid COVID-19 surge
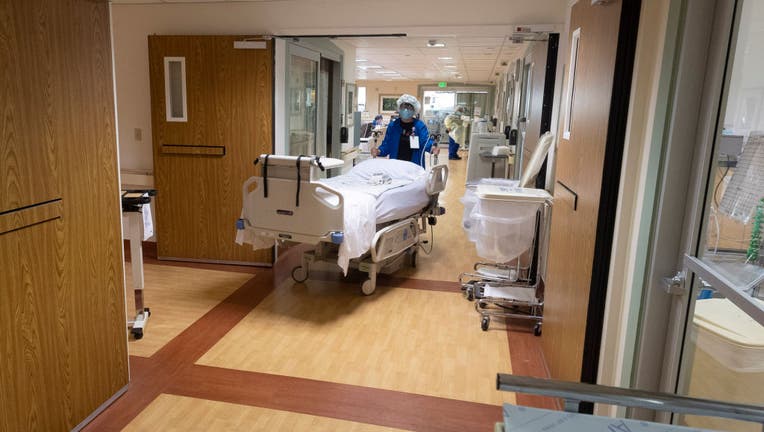
(Photo by Paul Bersebach/MediaNews Group/Orange County Register via Getty Images)
SANTA ANA, Calif. - With COVID-19 hospitalizations at a high, Orange County hospitals were being directed Thursday to implement surge plans and cancel elective surgeries in response to a "crisis" situation that could cause the emergency medical system to "collapse."

OC hospitals implement COVID-19 surge plans
Orange County hospitals are now implementing coronavirus surge plans as cases continue to spike throughout Southern California.
On Wednesday, the Orange County Health Care Agency reported that the total number of hospitalized coronavirus patients had surged by 28, reaching a total of 974, including 239 people in intensive care units, just a half-dozen shy of a mid-July peak and up from 235 on Tuesday.
The HCA also reported 2,613 new coronavirus diagnoses on Wednesday.
Orange County is expected to receive its first round of the Pfizer vaccine on Dec. 15, health officials said.
RELATED: Orange County preparing for first Pfizer vaccine shipment
The number is a single-day record, although Orange County CEO Frank Kim said a backlog of test results from the state may have contributed to the sharp increase.
The county's cumulative case count stands at 93,126, but no new fatalities were reported and the death toll remained at 1,633.

(Getty Images)
Late Wednesday night, the HCA sent a letter to hospitals, ambulance providers and 911 paramedic providers, saying the county's health care system is "now in crisis" due to the surge in COVID patients, with more hospitals requesting diversion of ambulances to other medical centers due to patient volumes.
According to the letter, "This results in dangerous delays in initial patient assessments to ensure they don't have an emergency medical condition. Hospitals are overwhelmed with admitted patients to both the floors and the ICUs. At the current rate of deterioration, the EMS system may collapse unless emergency directives are implemented now."
The letter from Dr. Carl Schultz, HCA's EMS medical director, urges hospitals to activate surge plans, establish alternate treatment areas in emergency departments to expand capacity, cancel all elective surgeries, apply for state waivers in support of surge plans and establish emergency operations centers.
RELATED: Stay up to date on all coronavirus-related information
"To those facilities that have activated these initiatives, all healthcare partners and the citizens of Orange County are grateful," Schultz wrote. "To those who have chosen not to take this painful but necessary actions, there is still time, but you must act now."
Schultz's letter was a recommendation at this time, but it could precede an order from Dr. Clayton Chau, the county's chief health officer and director of the Health Care Agency, Orange County Supervisor Lisa Bartlett said.

OC hospitals told to add space, cancel surgeries
With COVID-19 hospitalizations at a high, Orange County hospitals were being directed to implement surge plans and cancel elective surgeries in response to a crisis' situation that could cause the emergency medical system to collapse.
Bartlett, who is also on the Orange County Fire Authority board, said ambulance services are experiencing delays in transferring patients.
"When you get a 911 call and a patient is coming into the ER and they call the ERA and they say they're completely full and we're referring you to another hospital there could be a 15 to 20-minute delay getting that patient into another hospital,'' Bartlett said. ``When you get a 911 call, time is critical and every minute makes a difference."
Bartlett said the county is likely now just experiencing a surge of cases from Thanksgiving.
"It further emphasizes my point that it's not things like outdoor dining at restaurants causing Covid surge. It's small- to medium-sized gatherings," Bartlett said.
The county's percentage of available ICU beds dropped from 13% Tuesday to 11.2% Wednesday, but according to a new state metric for "adjusted" ICU bed availability, the rate is at 4.9%, according to the HCA.
Kim said the "adjusted" case rate essentially reflects the estimated number of beds available for COVID-19 patients when factoring in the number of beds needed for patients without the coronavirus.
The county has 53% of its ventilators available.
RELATED: Interactive Map of Coronavirus Cases
The 11-county Southern California region's available ICU capacity diminished to 9%.
Orange County's adjusted daily case rate per 100,000 rose Tuesday to 30.3, up from 22.2 last week, with the positivity rate increasing from 8.8% to 10.6%.
The county's Health Equity Quartile Positivity Rate, which measures the cases in highly affected, needier parts of the county, rose from 13% last week to 16.2% this week.
All of the county's metrics now fall within the state's most- restrictive, purple, tier of the four-tier coronavirus monitoring system.
RELATED: More California counties on lockdown as COVID-19 skyrockets
County officials are again focusing on a surge in coronavirus cases in skilled nursing and assisted living facilities, Kim said.
There are two-dozen skilled nursing facilities in the county that have reported two or more cases of COVID-19 in the past two weeks, and 22 assisted living facilities with two or more cases in the past 14 days.
County officials were asked to provide personal protective equipment, more training or staffing to help curb the spread of COVID-19 in those facilities, where the main reason for the spread is likely from employees who contract the virus off-site, Kim said.
Sixty-four residents signed up at Tuesday's Orange County Board of Supervisors meeting to comment on the state's regional stay-at-home order triggered last week when Southern California's intensive-care unit bed availability dropped under 15%.
Most pleaded for the county to ignore it.
County Supervisor Andrew Do asked Dr. Clayton Chau, the county's chief health officer and director of the Health Care Agency, to reiterate the county's lack of control over the stay-at-home orders.
The board unanimously approved a resolution requesting more local control over regulating COVID-19 measures.
Supervisor Don Wagner, an outspoken critic of Gov. Gavin Newsom's management of the pandemic, said the supervisors cannot ignore orders from Newsom. But Wagner railed against state officials, who, he said, were "playing us for fools, saying you guys have to follow these rules, and they're making up the rules as they go along."
Wagner pointed to instances in which Democratic political leaders flouted coronavirus regulations, including Newsom attending a gathering at a top Napa Valley restaurant, and said it was evidence that they did not believe the rules were necessary to curb the pandemic.
"They don't follow the rules because they don't have faith in the rules as necessary or as helpful," Wagner said.
Orange County Supervisor Lisa Bartlett, who co-sponsored the resolution with Wagner, said, "Local control is the best way to go."
Bartlett decried a "heavy-handed, one-sided approach from Sacramento," and said counties must get out of a cycle of opening-and-reopening the economy. "They can't keep shutting them down again. It's detrimental, it's terrible for the workforce to be hired and fired."
Do said he supported the resolution, but wanted to strip the politics out of it.
Outgoing board Chairwoman Michelle Steel, who was elected last month to Congress but has not resigned her county post, criticized Newsom's order and asked the county CEO to issue a memo on the consequences of ignoring the stay-at-home regulations.
Chau told the supervisors that the county is expecting about 25,000 doses of the first round of vaccines to be doled out nationwide. If the vaccines are approved by the federal government this week, the county could receive its first portion by Dec. 15 to be administered to critical health care workers, Chau said.
Vaccines for the general public are expected in the late spring or early summer, he said.
Do said the county's new home test kits have been made available to all residents. Previously, the saliva-based home test kits were first distributed to residents in Anaheim and Santa Ana, the county's hot spots for coronavirus.
For the first time, all county supervisors wore masks through the duration of the meeting. That was because of a new guideline from CalOSHA directing businesses and organizations to instruct employees to wear masks, Kim said.
Get your top stories delivered daily! Sign up for FOX 11’s Fast 5 newsletter. And, get breaking news alerts in the FOX 11 News app. Download for iOS or Android.

